Meningitis is the inflammation of the membranes that surround the brain and spinal cord. It is most common in babies, young children and teenagers but can affect anyone of any age or gender. It appears to be seasonal illness with peaks coming in January though to March. Some of the same bacteria that causes Meningitis can also cause Septicaemia which is also known as blood poisoning. Meningitis is a very fast moving illness and if not treated quickly can be fatal in five to ten percent of cases where treatment has already been administered. Both the viral and bacterial strains can be highly contagious so it is important that anyone who has been in close contact with a patient gets treated too. As well as close contact Meningitis is transmitted through the droplets released when coughing and sneezing.
Symptoms can begin with a cold or the flu virus which then leads onto the more extreme illness of Meningitis. The bacterial strain is usually more severe and severity can also vary based on your age.
Viral and bacterial Meningitis in small infants and children can present as pale skin, a decreased appetite, irritability and confusion, sleepiness and being difficult to wake. Floppiness and lethargy. Also a high fever may be present. In any infant under the age of three months a temperature of thirty eight degrees and over should be seen by a medical professional. Due to muscle pain and headaches the child may not like being picked up and held. They could also have a high pitched cry along with fast breathing or appearing breathless.
These symptoms can appear in any order and not all of them may be present in every case.
In adults viral Meningitis can present with, a severe headache and a stiff neck. A common test for potential patients is to ask them to place their chin to their chest. Many people believe that if they can perform this test then the illness is not Meningitis. Along with the headache there is sometimes an extreme sensitivity to light, which could lead the person to believe they have a migraine. Nausea and vomiting are other common symptoms and often patients may believe they are just suffering from a stomach virus. Sleepiness, lethargy and a decreased appetite are also common symptoms.
There is no specific treatment for the viral strain of meningitis but rather the medical professionals try to treat the symptoms, for example paracetamol to help lower the fever and fluids to help with dehydration, as antibiotics do not work on viral infections. Patients will normally recover in about ten days, normally with no need for admission into hospital.
Bacterial Meningitis tends to be a lot more severe and fast moving. Symptoms will normally come on extremely quickly. The symptoms mirror a lot of the same ones as with viral meningitis such as headaches, stiff neck, sensitivity to light and nausea and vomiting
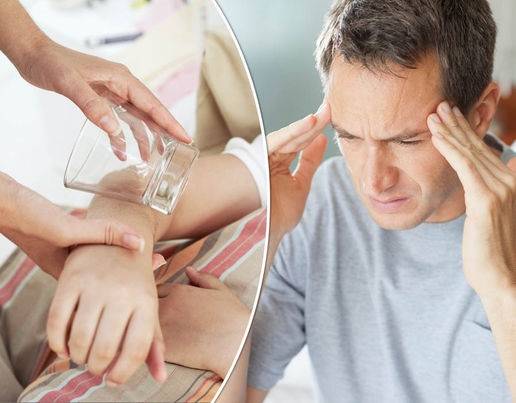
With the bacterial strain both adults and children may also develop a purple rash. This may not be present in all cases though. This rash is caused by the meningococcal septicaemia, meaning that the infection has entered into the bloodstream. It can be one of the last symptoms to appear so do not wait if you think someone under your care potentially has Meningitis. This distinctive rash appears like pin pricks and is the blood vessels becoming damaged as the bacteria in the bloodstream multiply rapidly and release endotoxins (poison.) The rash is non blanching, meaning that it does not disappear when placed under pressure. To test for this rest –
Using a glass gently place it over the rash.
Move it around slightly, the spots may disappear slightly to begin with and then reappear.
If the spots do not fade or disappear to begin with and then reappear then this is a medical emergency and medical help should be sought immediately by calling the emergency services.
Other signs of Septicamia that accompanies meningitis are
Cold hands and feet, even when a fever is present.
Severe joint and muscle pain,
Rapid breathing,
Stomach cramps and diarrhoea.
Bacterial Meningitis and Septicaemia will need to be treated in hospital. It will usually be diagnosed with a blood test to check for bacteria and infection markers. A lumbar puncture will be taken, this is where a sample of spinal fluid is collected and then tested for infection and also a CT scan may be done to check for any swelling in the brain.
Treatment will normally begin before the diagnosis is confirmed as time is critical and early intervention is key for survival. As well as antibiotics, fluids and oxygen will also be given. Sometimes also a steroid medication will be given to reduce any swelling in the brain.
Neonatal meningitis is where the infection affects babies in their first weeks of life. The most common cause of neonatal meningitis is a bacterial infection of the blood called bacteremia or Group B Streptococci. For example, if a mother has undiagnosed Group B Strep in pregnancy, the infection could then be passed onto the baby during the labour and delivery. According to the Birth Injury Claims specialists 0.4 babies out of 1000 live births will develop Neonatal Meningitis.
Symptoms are similar to meningitis in older children and adults but may also include a bulging fontanelle, jaundice, seizures and sunset eyes, which is the downward gazing of the eyes. They may also have a weak cry. Obviously babies cannot communicate how they are feeling so if any or these symptoms develop then this should be reported to your midwife, doctor or a Nurse.
Complications such as hearing loss, epilepsy, paralysis, memory loss and vision loss can occur as a side effect to the infection. In severe cases to stop the infection spreading amputation of limbs is needed.
There are several vaccinations now available for meningitis which are given as routine to children in their early years. Although these do not cover every strain, since the start of these vaccinations, the cases of bacterial Meningitis have halved in the United Kingdom.


Comments are closed.